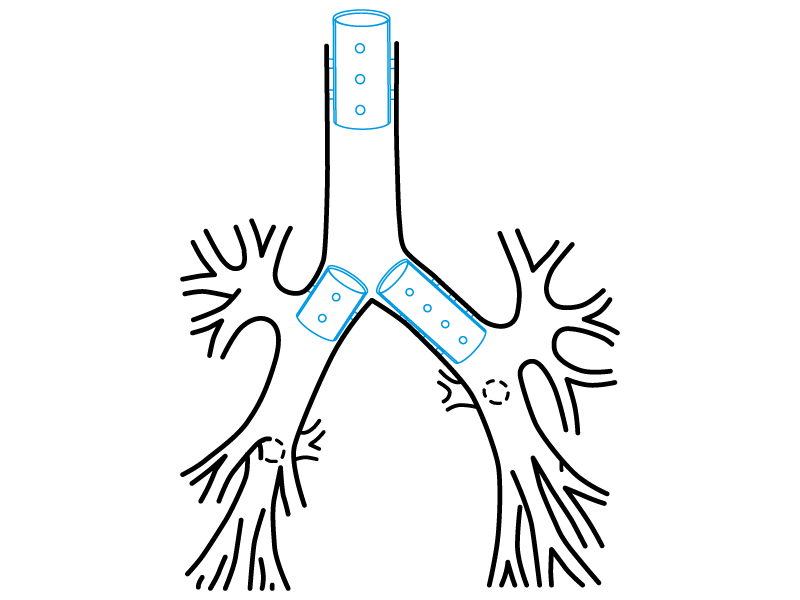
Subglottic Stent
Code SG

Description
The subglottal stent presents an 8 mm section on its proximal edge where its wall’s thickness is reduced. Throughout this section, its normal wall, of 1.5 mm, reduces its thickness gradually until it ends.
This wall’s thickness decreasing achieves, on that edge, a surface of low resistance on the stent. It is meant to occupy the subglottic region, close to the vocal chords. This design allows the stent deformation during the laryngeal movements and the glottal dynamic during swallowing and phonation.
The stent fixation on the trachea will be carried out by the remaining walls of the prosthesis, of a standard shape and width.
The use of the subglottal stent can be preferred for other locations such as the middle or lower trachea or even in the source bronchi, replacing a classical stent.
As it can be understood, when this stent is implanted in the source bronchus, with its “subglottal” edge in the proximal direction, the transition from the bronchial mucosa to the stent inside will be very smooth, without the “step” that accompanies the classical stent. That could help to reduce the turbulence of the air flow and the secretions impaction.
- Tracheal stenosis close to the subglottis
- All indications from every tracheal and bronchial stent
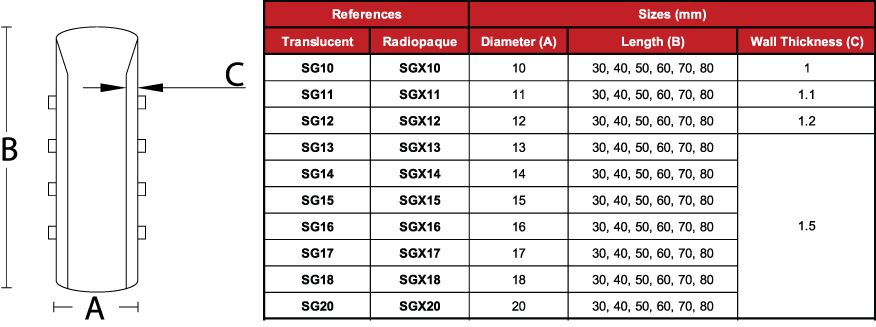
Due to the characteristics of the production process, the
measurements of the devices can vary by +/- 2%
- Medical grade silicone
- Bevelled edges to prevent granulomas
- Spur system to prevent migration
- Removable
- Surface of maximum softness to avoid adherence of secretions
- Transparent or Radiopaque
Introduction technique:
The procedure is the same that the described for tracheal or bronchial stents.
Naturally, when the stent is introduced inside the charger or inside the bronchoscope or tracheoscope, you will have to make sure that its “subglottal” end (the one with thinner wall) remains on a proximal position (or cephalic). In other words, it must be positioned in the surgeon’s direction. This is the only way in which the stent, once freed inside the airway, could achieve all its duties that make it different from the rest.
The stenosis length and diameter must be carefully determined, in order to get the suitable stent with the right dimensions.
The final distance between the vocal chords and the stent must be equal or greater than 2 mm. Keep in mind that the distances inside the affected trachea are difficult to estimate due to the fact that they will change when the patient acquires the standing position.
A major drawback is added in the distances determination within the airway because of the muscular recovery after the metabolism of the relaxants used in the anaesthetic act.
Remember that, in addition, you will confront the length modifications that can occur in the trachea after being submitted to tractions and elongations because of the dilatation manoeuvres carried out with the rigid tools.
Even though some or all of these circumstances can be present in every tracheobronchial recanalization procedure and implant, they gain a crucial interest in the diseases that have a subglottal location. This is due to the precision that is necessary for leaving the stent only a few millimetres close to the vocal chords. This will require the best of skills and knowledge.
Removal:
We will proceed to the intubation with a rigid tracheoscope or bronchoscope.
The stent must be taken by its edge with an alligator forceps with the correct steadiness. Depending on the time the device had been inside the airway, the stent border can be confused with the bronchial wall.
After holding the stent, rotate the forceps 360º. By performing this movement the stent will bend, reducing its diameter and losing its radial resistance to compression.
Then manipulate the forceps to remove the prosthesis and the endoscope. If you prefer, the stent end can be introduced inside the bronchoscope. With this manoeuvre the vocal chords are protected during the removal.
- When an increase in secretions is detected, perform frequent nebulisations with a warm isotonic saline solution.
- Treat cavities and take care of your oral hygiene.
- Endoscopic controls must be performed following the doctor instructions.
The product should not be reused because this can cause cross contamination.
A sterile non-bioabsorbable tubular device intended to be implanted into the trachea and/or a bronchus/bronchiole to maintain luminal patency, typically used in cases of obstructions/stenoses, fistulae, tumours, scarring, surgical resection and anastomosis, or pulmonary transplantation. It is made entirely of a synthetic polymer(s) [e.g., silicone] and may have various designs (e.g., semi-soft continuous tube, covered or non-covered mesh structure, straight or branched configuration) intended to conform to the endotracheal/endobronchial surface. It may be expandable in situ (e.g., self-expands) and disposable devices intended to assist implantation may be included.
46977